
Sara Riggare, Queen of self-tracking
When I met Sara
Or how science got personal
14th of March 2022
Part 1. To track or be tracked
I first met Sara on Twitter in 2019 in a discussion on the Personalized Parkinson’s Project (PPP; Bloem, 2019). I had enrolled and had just started wearing the accompanying “self-tracking watch”. Sara insisted to the principal investigator prof. dr. Bas Bloem that the things that would be tracked should be of importance to the people wearing the watch. I remember saying I was OK that the watch was first tested for research purposes. Little did I know then that during the two years of wearing the watch 24/7 myself, I would live through her wise words from first-hand experience.
On the day the watch was calibrated to my bodily signals and symptoms, I had already asked questions about what we would get back from the watch. Apart from the fact that it was a beautiful watch, the only thing I could learn from it was the time of the day, which has little to do with my Parkinson’s. So I suggested that the least we could get, was an insight into the steps we took on a daily basis, information about our sleeping pattern, our heart rate. I was told that an update of the software that would provide us with more personalised information would shortly follow! I asked and mailed about it several times afterwards, but – supposedly to the joint frustration of both the principal investigator and myself – in the two years I participated in the study this software update never came.
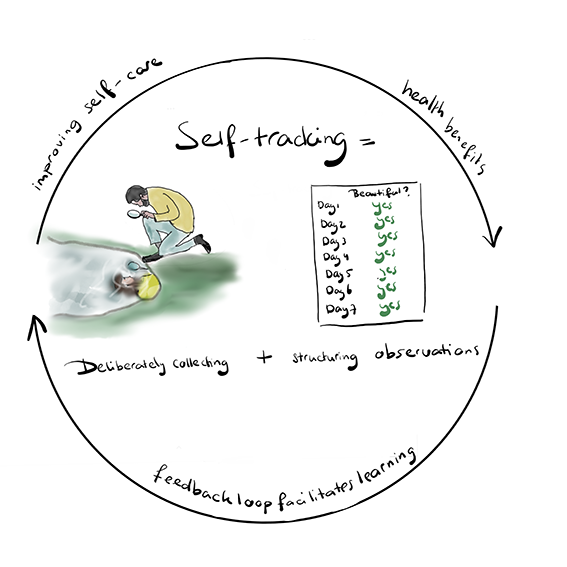
Sara defines self-tracking ‘a process of deliberately collecting and structuring observations about one’s own life’. It can be used as a method for data collection in personal science – with the intention to improve self-care – or it can be used as a method to gain insights at group level.
Proving Sara right
Another software update did arrive. It was an update where one has to do UPDRS-like tests like finger tapping, opening and closing one’s hand as fast as possible, tapping with one’s foot on the floor, balance, etc. This truly flashy update made my motivation drop. It’s no fun seeing how you can’t tap your fingers or foot, especially when these are not the problems you worry about in daily life. It had been my problems with multitasking and keeping an oversight in crowds that had forced me to rethink my job description.
The thing that struck me most during the PPP was that it was ‘not possible to return research data at an individual level’ because ‘such information has not yet been validated for clinical purposes’. I understand that returning all data is not for everyone. But ‘not possible’ is really too easy. So yes, two years into the game of ‘self-tracking’ without getting the feedback to learn from it, I had to say that Sara had been completely right. Clinical studies should track the things that matter most to patients and allow these ‘essential volunteers’ – as Lewis describes us – to learn from the data. Otherwise, it’s just a ‘permission to be tracked’, surveillance even. Which is disconcerting for those who want to know as much about their disease as I do.
Don’t get me wrong: it’s not that I don’t want to contribute to making the future better for all people who are going to get Parkinson’s. I have worn a research watch 24/7 for 2 years to substantiate these intentions. I just think that a win-win outcome could have been and should have been designed from scatch, taking the experience of data donors as seriously as developing possible treatments for their future counterparts.
A major challenge is that the views of clinicians and researchers on what is important in order to help persons with PD are often different from what persons with PD consider most important. This means that we need to ensure that new technological applications should be developed that address the issues that patients find important rather than the ones clinicians prioritize | Sara Riggare
Part 2: Sara’s journey
I see my neurologist twice a year, about half an hour every time. That’s one hour per year in healthcare for my Parkinson’s disease. During the same year, I spend 8,765 hours in selfcare, applying my knowledge and experience together with what I get from my neurologist to manage a difficult condition as best I can. I am not saying I want more time in healthcare. I really don’t think I need more time with my neurologist. However, I am saying that healthcare needs to acknowledge the work we patients do in selfcare and also start working to make use of our observations for their own knowledge. Just imagine what we could achieve if we start working together – as equals with different but complementary areas of expertise! | Sara Riggare


Sara in Sweden
In order to be taken seriously by academic researchers, you have to be a researcher yourself | Sara Riggare in her thesis
Making science personal
By the time I was diagnosed in 2018 and had subsequently enrolled in PPP, Sara already was an experienced patient, patient advocate, and patient researcher (Riggare, 2020). Her Parkinson’s diagnosis was in 2003 at the age of 32 and she had already had symptoms since she was 13.
Parkinson’s disease is a complex, multifaceted, syndrome with a range of causes and recognisable clinical presentations. At present, no therapy can slow down or arrest the progression of Parkinson’s (Bloem, 2021). All we currently have is a symptomatic treatment, masking some of the many symptoms while possibly generating others. Sara had long come to the understanding that, considering the highly individual and fluctuating nature of Parkinson’s, people with Parkinson’s would very likely benefit from tracking their own symptoms and adjusting treatment accordingly.
Instead of using self-tracking to improve her selfcare only, Sara decided she wanted to help build the evidence base for what works in selfcare for other persons with Parkinson’s as well. To do so, she knew she would have to become a researcher herself. To truly bridge the gap, she knew she would have to publish her findings ‘where they are’, in journals where researchers tend to look. Sara had the drive, talents, and skills to pursue and further the field of patient-led personal science. She embarked on a journey to improve understanding of what personalised care – selfcare – actually means for persons with Parkinson’s like herself.
One size doesn’t fit all in the management of Parkinson’s Disease | Sara Riggare in her thesis
5 images of personal science
Sara defines personal science as ‘The practice of exploring personally consequential questions by conducting self-directed N-of-1-studies using a structured empirical approach”, complementary to conventional clinical research. In this type of research the researcher and research participant are one and the same. Personal science can answer the question: What works for me?
Resistance
in 2012 Sara started to pursue a PhD in patient-led personal science where the researcher and research subject are the same. She obviously was defying the status quo and met with resistance. The resistance that struck her most was from a fellow researcher who said: “But Sara, why would patients want to do research on themselves anyway? Wouldn’t it be better if you all just give your data to a proper researcher”?
Sara just kept on following her hopamine. She had published two articles to set two examples: She studied the effects of her medication on her finger-tapping abilities – measured via an app – and found a dip in finger function around the time of her second medication dose of each day. In another study, she studied the effect of nicotine administered via an e-cigarette on levodopa-induced dyskinesia. Only to show that work done by patients on a daily basis can enhance their understanding of their disease. Her whole point being to create feedback loops and facilitate learning, first for herself and second in encounters with clinicians.
To investigate the transferability of using self-tracking in personal science, Sara designed a survey for people with PD in Sweden. Sara found out that transferability had several challenges. First, you have to know enough about PD to know what and how to track. Second, the benefits and burdens of self-tracking have to be balanced. Focusing on symptoms too much may increase the felt burden. One of her participants provided a way out: Why not focus on what makes a good day instead?
Still the resistance didn’t keep silent. When Sara handed in her application to defend her PhD thesis in 2018, the ethical committee at the Karolinska Institute where she started her PhD didn’t allow her to finish. It was then that Prof. Dr. Bas Bloem and Dr. Martijn de Groot adopted her work at the Radboudumc in Nijmegen, the Netherlands. By writing a paper about the ethics of self-tracking (Riggare, 2021) she was back on track.
The present discussion about personal science raises an almost philosophical issue about science in general, namely that the purpose of all research should ultimately be to benefit not the groups that were studied in a particular study, but rather individuals living with a chronic condition like PD | Riggare, 2021
Final part: Three rebels with a cause
On the 25th of March 2022, Sara will finally put an end to the resistance she met. She will be the first person to defend a PhD thesis that was based on self-research. I have the honor to be on the opposition committee even though I didn’t finish the PhD I once started. Here, Bas Bloem didn’t only fight for Sara, he walked his talk for me too, for which I’m more than grateful. He had to write a letter to the dean stating that one could argue that the patient perspective should be taken very seriously, also during the public defense of a PhD thesis.
Three years after our brief encounter on twitter, Sara, Bas and myself (and others ;-)) meet again at the public defense of Sara’s thesis. During a defense, challenging each other’s assumptions is all in the game. In fact, it IS the game. Opinions are not seen as ‘criticism’, are not taken personally, but exactly as they are meant: A reminder that we all have a role in complementing each other’s blind spots, making sure that the things we strive for don’t get lost in translation, making sure that science gets as personal as it may possibly get.
So looking forward.
I am VERY happy and proud to be able to announce that my PhD thesis is now available! Huge thanks to supervisors supreme @basbloem @grootm75 @MariaHagglund https://t.co/33j9lCPLKk
— Sara Riggare 📌 (@SaraRiggare) January 21, 2022
Don’t forget to tune in on the 25th of March! Apart from Sara defending her thesis, with my think-alike Mariette Robijn as one of her paranymphs, there will also be an online personal science symposium from 3.00 – 5.00 pm CET. Several speakers will share their views on this emerging field of personal knowledge creation, including Bas Bloem, Sara Riggare, Jakob Eg Larsen, Thomas Blomseth Christiansen and Gary Wolf. The program will be an interesting and inspiring mix of keynotes, show and tell, round table discussion and a special unveiling… You can register here.
Sparks
Sources
- Bloem, B.R., Marks, W.J., Silva de Lima, A.L. et al. (2019). The Personalized Parkinson Project: examining disease progression through broad biomarkers in early Parkinson’s disease. BMC Neurol 19, 160. https://doi.org/10.1186/s12883-019-1394-3 (Open Access)
- Bloem, B. R., Okun, M. S., & Klein, C. (2021). Parkinson’s disease. The Lancet, 397(10291), 2284–2303. https://doi.org/10.1016/s0140-6736(21)00218-x (Closed Access)
- Lewis, M.A.(2021). Return of Results to Patients: A Gesture of Respect and Responsibility. Journal of Immunotherapy and Precision oncology. https://doi.org/10.36401/JIPO-21-X7 (Open Access)
- Riggare, S., & Hägglund, M. (2018). Precision Medicine in Parkinson’s Disease – Exploring Patient-Initiated Self-Tracking. Journal of Parkinson’s disease, 8(3), 441–446. https://doi.org/10.3233/JPD-181314 (Open Access)
- Riggare, S., Patient researchers — the missing link?. Nat Med 26, 1507 (2020). https://doi.org/10.1038/s41591-020-1080-4 (Closed Access)
- Riggare, S., Hägglund, M., Bredenoord, A. L., de Groot, M., & Bloem, B. R. (2021). Ethical Aspects of Personal Science for Persons with Parkinson’s Disease: What Happens When Self-Tracking Goes from Selfcare to Publication?. Journal of Parkinson’s disease, 11(4), 1927–1933. https://doi.org/10.3233/JPD-212647 (Open Access)
* This was part IV of a series of blogs in which I put a Parkyvist in the spotlight. In my definition, a Parkyvist is someone who has a diagnosis of Parkinson’s disease and who noticeably uses his/her talents to make a positive contribution to the Parkinson community as a whole.
- Part I: Benjamin Stecher
- Part II: Ruud Overes
- Part III: Kevin McFarthing
- Part IV: Sara Riggare




